Why Stomach Acid Is Good for Us
LifeSource Natural Foods | Posted on |

Ask the average person (including the average doctor) what causes heartburn and they’ll answer “too much acid” aka “hyperchlorhydria.” However, too much acid is far less common than having too little acid. It’s actually quite rare. So then, why do so many people experience heartburn, reflux, ulcers, poor digestion, and poor nutrient absorption?
The answer is surprising: Too little stomach acid.

The reasons for low stomach acid are numerous, ranging from stress to aging to poor diet, food sensitivities, eating too quickly, overuse of antacids and proton pump inhibitors (PPIs), and the “I’ve got to alkalinize my body” craze. We have been conditioned to view stomach acid as the enemy, so we go to great lengths to suppress it even further, without understanding the damage we do to ourselves when we do so. Let’s take a look at some basics.
Why is stomach acid necessary?

What is its function? Stomach acid does several things. It breaks down proteins, kills pathogenic bacteria and other microbes that might be lurking in our food, triggers the release of other digestive enzymes from the liver, gallbladder, and pancreas, and it breaks down vital minerals like calcium and iron so that they can be absorbed rather than excreted. It’s also responsible for ensuring that the Lower Esophageal Sphincter (LES,) which is the door that leads from the esophagus to the stomach, stays closed so that acid and food do not come back up the esophagus.

The optimal pH of the stomach is between 1.5 to 3 on the pH scale. Zero is the most acidic and 14 is the most alkaline. Battery acid is at 1 on the pH scale. Lemon juice around 2.5, and vinegar around 3. So, we want our stomach acid to resemble something like pure lemon juice or apple cider vinegar. That’s pretty acidic.
What happens when we don’t have enough acid?
First, the LES doesn’t get the signal to close. Without enough acid, the door at the top of your stomach stays wide open. When you eat, the food doesn’t break down. It just sits there, rotting and fermenting, until gravity eventually takes over. Meanwhile, gas is being produced which pushes the food, and whatever little acid is present, up into the esophagus, leading to heartburn and, in extreme cases, GERD (GastroEsophageal Reflux Disease.)

Second, the stomach, liver, gallbladder, and pancreas don’t receive the signal to do their jobs properly. Acid tells the stomach to convert inactive pepsinogen into active pepsin so that it can break down proteins into absorbable bits before they enter the small intestine.
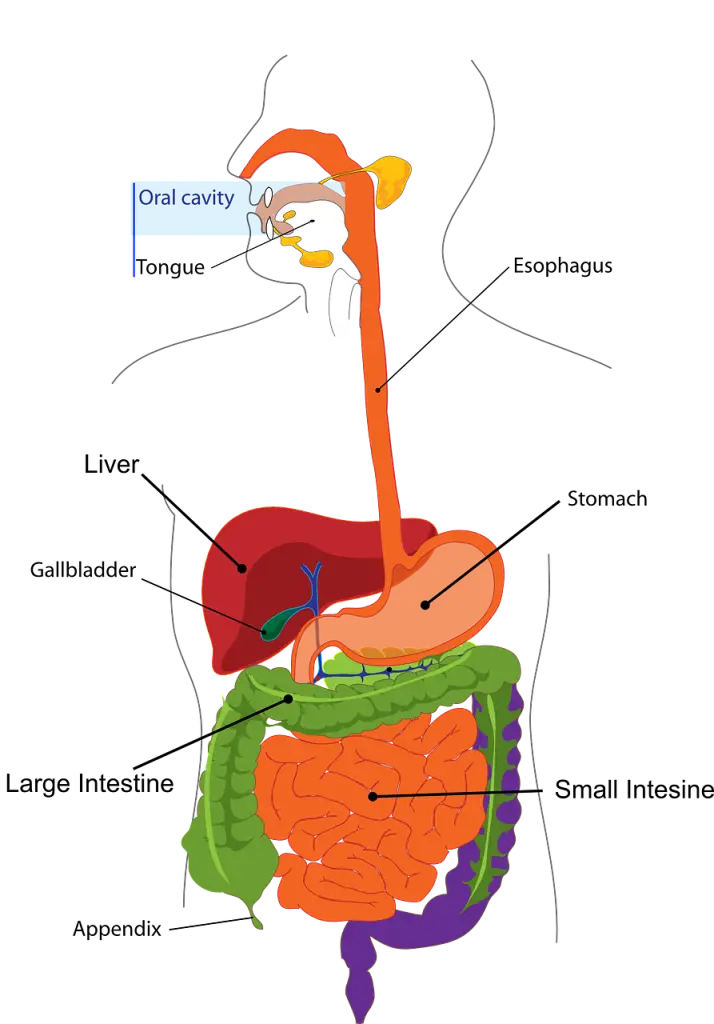
Acid tells the liver and gallbladder to release bile which is needed to emulsify (break down into small particles) fats so they can be digested properly. Lipase, which is the enzyme that digests fat, is produced in the pancreas, but it won’t be secreted properly without the acid trigger. The pancreas also needs the acid trigger to produce other protein digesting enzymes to enable nutrient absorption, as well as creating sodium bicarbonate to neutralize the acidified proteins in the stomach known as chyme before it goes into the small intestine. Without that sodium bicarbonate, the chyme will burn the small intestine.

Third, undigested proteins will go into the small intestine where they cannot be further broken down or their nutrients absorbed. This causes intestinal distress, inflammation, dysbiosis, and, eventually, “leaky gut” which means you’re not getting the nutrients you need, but are susceptible to having those undigested proteins, as well as bacteria, leak into your bloodstream causing histamine and immune responses against the foreign invaders.
At the extreme end of this dysfunction is the potential development of an autoimmune response where your body starts attacking random proteins in your body (like your joints, thyroid, or other organs,) rather than just the foreign invaders.
Lastly, without sufficient acid you cannot cleave minerals into smaller, more absorbable particles. They won’t be in useable bits, so your body just excretes them. This is one of the primary reasons why people who take antacids or PPIs (proton pump inhibitors) long term end up with mineral deficiencies, muscle cramps, anemia, and osteoporosis. They’re simply not getting the minerals they need from food or supplements because their body doesn’t have what it needs to make them bioavailable.

So, how can we optimize proper stomach pH to improve our digestion while lowering incidents of heartburn and acid reflux?
How can we improve our digestion?

One of the best places to start sounds a lot like advice you’d get from grandma: Slow down. Don’t eat on the run. Don’t eat while stressed or distracted. Sit down and focus on eating. Chew, chew, chew your food properly. Put your fork down between bites. Consume nutritious foods and avoid sugar, sodas and other junk.

Some people find that priming the digestion prior to meals is very helpful in activating the enzymes needed. You can do this by using digestive bitters or drinking a bit of lemon water or apple cider vinegar in water. Acidifying the stomach just prior to eating or taking mineral supplements will increase your ability to digest properly. Some people find that taking their iron or calcium supplement with orange juice helps them to better absorb the minerals.

Digestive enzymes that contain HCl (hydrochloric acid) are very helpful. For people who are very sensitive, or who have a weak LES, taking DGL (deglycyrrhizinated licorice) to protect the mucosal lining of the stomach and esophagus is helpful. It’s especially useful for people who are titrating off of PPIs.
A word about proton pump inhibitors (Prilosec, Prevacid, Protonix): Proton pumps don’t just exist in the stomach. They exist in almost every cell in the body. Taking a PPI to reduce stomach acid doesn’t just affect digestion. It affects ALL proton pumps throughout the body, including those responsible for cellular energy, by interfering with ATP production and storage, reducing nitric oxide production which is necessary for proper blood vessel dilation, interfering with brain cells’ ability to communicate with each other, as well as a risk of an increased buildup of amyloid plaque which raises Alzheimer’s risk. Stopping PPIs suddenly will cause a painful and discouraging rebound effect, and it should not be attempted without communicating your intention with your doctor and working with them to formulate a plan to do so safely.

Several other herbs are beneficial demulcents, which protect the mucosal lining of the esophagus, stomach and gut, allowing them to heal. These include marshmallow root, slippery elm, aloe vera, and mastic gum. Mastic gum, especially when used with zinc l-carnosine, encourages healing of the mucosal lining of the stomach and gut, as well as possibly inhibiting the ulcer causing bacteria H. Pylori and healing damage it causes. Raw cabbage juice contains nutrients which have been shown to heal ulcers in both the stomach and the gut.

These supplements and nutrients can be incorporated into an overall plan to optimize stomach acid, protein digestion and nutrient absorption, while minimizing discomfort.

For more in depth info, with citations to detailed studies, I highly recommend the book “Why Stomach Acid Is Good For You: Natural Relief from Heartburn, Indigestion, Reflux and GERD” by Jonathan V. Wright, MD and Lane Lenard, PhD.



4 Comments
Applecider vinegar nutrilizes stomach acid
Hi! Can I take apple cider vinegar with meals even if I am taking zinc carnosine? Or should it be on or the other?
I have the same question. I wonder if I can take them both at the same time?
Sarah, Kimberly,
I wish I had an answer to your questions about this, but I am only a clerk in a grocery store, so I’m unqualified.
I would love to hear the answer you receive from a certified nutritionist, or medical professional.
Would you be so kind as to share the answer here for all who are interested? Thank you!